Introduction
Respiratory care is entering a new era in 2026.
Treatment is shifting away from broad-spectrum steroids and bronchodilators toward peptide-based precision medicine.
As asthma, COPD, cystic fibrosis, and pulmonary fibrosis become more prevalent, peptide therapeutics offer targeted solutions. These therapies address the underlying biology of lung disease while minimizing systemic side effects.
1. Peptide Therapeutics for Asthma and Allergy
For millions living with chronic asthma, peptide therapies are delivering new hope.
Rather than suppressing the entire immune system, these treatments quiet specific inflammatory pathways.
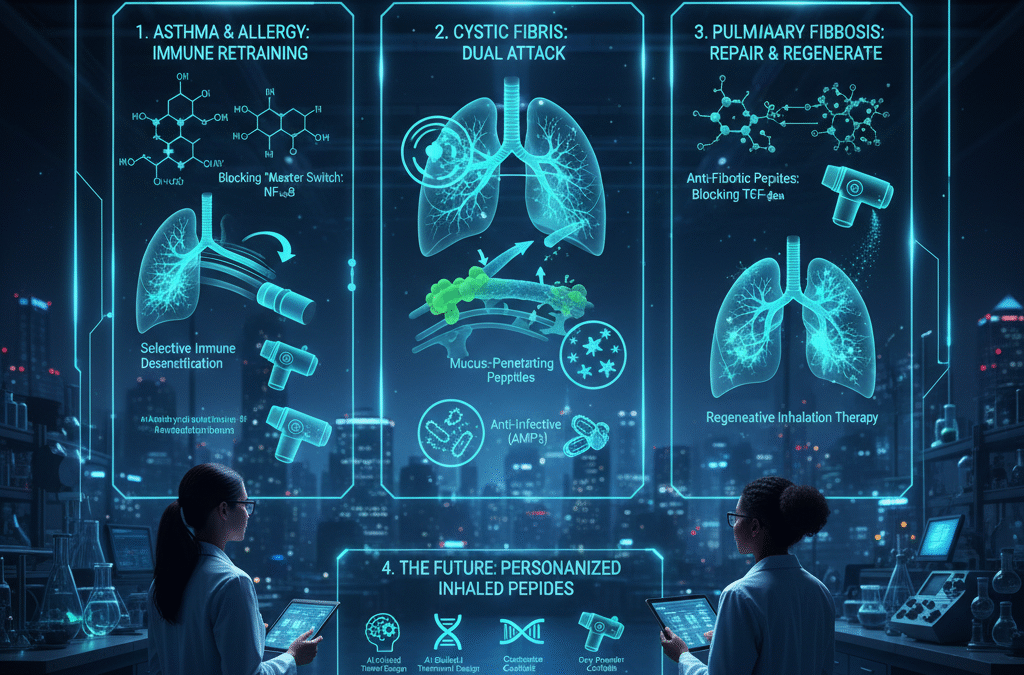
Blocking the Inflammatory “Master Switch”
Researchers are using peptides to inhibit signaling pathways such as NF-κB.
This pathway acts as a master regulator of lung inflammation. By blocking it, peptides reduce airway swelling at its source.
Selective Immune Desensitization
Peptide-based immunotherapy retrains the immune system.
Instead of exposing patients to whole allergens, clinicians use small peptide epitopes.
As a result, tolerance develops without triggering severe allergic reactions during treatment.
2. Breakthroughs in Cystic Fibrosis (CF)
In 2026, peptide therapy is transforming cystic fibrosis care. The focus now includes both mucus clearance and infection control.
Mucus-Penetrating Peptides
Thick, dehydrated mucus remains one of the greatest challenges in CF.
New synthetic peptides disrupt the molecular cross-links that trap mucus in the airways.
This thinning effect allows patients to breathe more easily and clear their lungs more effectively.
Anti-Infective Peptides
CF patients face constant threats from drug-resistant bacteria such as Pseudomonas aeruginosa.
Antimicrobial peptides (AMPs) physically rupture bacterial membranes, making resistance extremely unlikely.
As a result, AMPs are emerging as a critical new defense against chronic lung infections.
3. Pulmonary Fibrosis and Lung Tissue Repair
Idiopathic Pulmonary Fibrosis (IPF) has long lacked effective treatment options.
In 2026, peptide therapeutics are finally changing that outlook.
Anti-Fibrotic Peptides
Clinical trials are advancing for peptides that inhibit TGF-beta, the main driver of lung scarring.
By blocking this signal, these peptides may slow disease progression and enable natural repair mechanisms.
Regenerative Inhalation Therapy
Advanced delivery systems now allow peptides to be inhaled directly into the lungs.
Dry powder inhalers deliver repair peptides to the deep alveolar regions where damage is most severe.
4. The Future: Personalized Inhaled Peptides
Looking toward 2030, respiratory medicine is becoming increasingly personalized.
AI-Guided Treatment Design
In 2026, clinicians can use genetic markers and lung microbiome data to design custom peptide cocktails.
These therapies are delivered through smart inhalers that adjust dosing in real time based on lung function and inflammation levels.
Conclusion
The respiratory landscape of 2026 is defined by precision, biology, and personalization.
Peptide therapeutics are moving lung care beyond rescue inhalers and symptom suppression.
By targeting disease pathways at the molecular level, peptides offer a future where breathing becomes easier—and lung diseases are treated at their roots.